Abstract
The fluoroquinolone class of antibacterial agents are among the most frequently prescribed drugs, with utility in a broad range of bacterial infections. Although very useful agents, the fluoroquinolones as a class are associated with a number of adverse events, some with considerable clinical significance. In the past 15–20 years, tolerability concerns have led to restrictions on the use of the fluoroquinolones and, in some instances, the withdrawal of agents from the market.
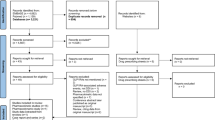
This review focuses on the safety and tolerability of levofloxacin, a third-generation fluoroquinolone, relative to other fluoroquinolones. A literature search was performed of the MEDLINE database encompassing the dates 1980–2009, using as keywords the drug names levofloxacin and concurrently marketed fluoroquinolones combined with the words ‘safety’, ‘adverse effect’ or ‘adverse drug reaction’, or the name of the specific adverse effect.
Adverse events commonly associated with the fluoroquinolones include gastrointestinal and CNS toxicity (most frequently headache and dizziness), as well as other adverse events including ECG abnormalities (for example QT interval prolongation), disrupted glucose metabolism, phototoxicity, tendon and joint disorders, hypersensitivity and skin disorders, and hepatic toxicity.
Package inserts for the fluoroquinolones in Europe and the US contain warnings regarding these risks. US package inserts also carry ‘black-box’ warnings regarding the risk of tendon rupture and joint disorders with these agents; however, there is a substantial body of evidence to indicate that there are marked differences in the tolerability profiles of the individual agents within the fluoroquinolone class. These differences may be explained, at least in part, by structural differences: all fluoroquinolones share a basic quinolone core, with differences in specific side chains underlying the adverse event relationships. Furthermore, many of the fluoroquinolone-associated adverse effects and toxicities occur more frequently in patients with pre-existing risk factors, or in certain subpopulations. Notably, package inserts for the fluoroquinolones carry warnings regarding use in the elderly, paediatric patients and patients with preexisting, or factors predisposing to, seizure disorders. Because of this, many adverse reactions with these agents could be prevented by improving patient screening and education. The recent withdrawal of gatifloxacin due to dysglycaemia makes it timely to review the safety and tolerability of the individual agents in this class. Overall, it appears that levofloxacin is relatively well tolerated, with low rates of clinically important adverse events such as CNS toxicity, cardiovascular toxicity and dysglycaemia.




Similar content being viewed by others
References
Linder JA, Huang ES, Steinman MA, et al. Fluoroquinolone prescribing in the United States: 1995 to 2002. Am J Med 2005; 118(3): 259–68
Ball P, Mandell L. Treatment of community-acquired respiratory tract infections. In: Hooper D, Rubinstein E, editors. Quinolone antimicrobial agents. Washington, DC: American Society of Microbiology Press, 2003: 227–43
Andriole VT. The future of the quinolones. Drugs 1999; 58 Suppl. 2: 1–5
King DE, Malone R, Lilley SH. New classification and update on the quinolone antibiotics. Am Fam Physician 2000; 61(9): 2741–8
European Medicines Agency. Public statement on Trovan/ Trovan IV/Turvel/Turvel IV (trovafloxacin/alatrofloxacin): serious, severe and unpredictable liver injuries. London: European Medicines Agency, 1999 May 25 [online]. Available from URL: http://www.ema.europa.eu/pdfs/human/press/pus/1577099EN.pdf [Accessed 2010 Mar 30]
US FDA. Trovan (trovafloxacin/alatrofloxacin mesylate): interim recommendations. Rockville (MD): US FDA, 1999 [online]. Available from URL: http://www.fda.gov/Drugs/DrugSafety/PublicHealthAdvisories/UCM053103 [Accessed 2010 Mar 11]
Levofloxacin (Levaquin) package insert. Raritan (NJ): Ortho-McNeil-Janssen, 2008
Ball P. Efficacy and safety of levofloxacin in the context of other contemporary fluoroquinolones: a review. Curr Ther Res Clin Exp 2003; 64(9): 646–61
Davis R, Bryson HM. Levofloxacin: a review of its antibacterial activity, pharmacokinetics and therapeutic efficacy. Drugs 1994; 47(4): 677–700
Lipsky BA, Baker CA. Fluoroquinolone toxicity profiles: a review focusing on newer agents. Clin Infect Dis 1999; 28(2): 352–64
Mandell L, Tillotson G. Safety of fluoroquinolones: an update. Can J Infect Dis 2002; 13(1): 54–61
Owens Jr RC, Ambrose PG. Antimicrobial safety: focus on fluoroquinolones. Clin Infect Dis 2005; 41 Suppl. 2: S144–57
Thomas RJ. Neurotoxicity of antibacterial therapy. South Med J 1994; 87(9): 869–74
Stahlmann R. Safety profile of the quinolones. J Anti-microb Chemother 1990; 26 Suppl. D: 31–44
Ciprofloxacin [Cipro] package insert. Kenilworth (NJ): Schering Corporation, 2009
Moxifloxacin [Avelox] package insert. Kenilworth (NJ): Schering Corporation, 2008
Kushner JM, Peckman HJ, Snyder CR. Seizures associated with fluoroquinolones. Ann Pharmacother 2001; 35(10): 1194–8
Van Bambeke F, Tulkens PM. Safety profile of the respiratory fluoroquinolone moxifloxacin: comparison with other fluoroquinolones and other antibacterial classes. Drug Saf 2009; 32(5): 359–78
Bellon A, Perez-Garcia G, Coverdale JH, et al. Seizures associated with levofloxacin: case presentation and literature review. Eur J Clin Pharmacol 2009; 65(10): 959–62
Hori S, Kizu J, Kawamura M. Effects of anti-inflammatory drugs on convulsant activity of quinolones: a comparative study of drug interaction between quinolones and anti-inflammatory drugs. J Infect Chemother 2003; 9(4): 314–20
Shrivastava MP, Makde SD, Paranjpe BD. Interaction of ciprofloxacin with diclofenac and paracetamol in relation to its epileptogenic effect. Indian J Physiol Pharmacol 1997; 41(2): 164–6
Bryskier A, Chantot JF. Classification and structure-activity relationships of fluoroquinolones. Drugs 1995; 49 Suppl. 2: 16–28
Domagala JM. Structure-activity and structure-side-effect relationships for the quinolone antibacterials [published erratum appears in J Antimicrob Chemother 1994 Nov; 34 (5): 851]. J Antimicrob Chemother 1994; 33(4): 685–706
Schmuck G, Schurmann A, Schluter G. Determination of the excitatory potencies of fluoroquinolones in the central nervous system by an in vitro model. Antimicrob Agents Chemother 1998; 42(7): 1831–6
Akahane K, Kato M, Takayama S. Involvement of inhibitory and excitatory neurotransmitters in levofloxacin- and ciprofloxacin-induced convulsions in mice. Antimicrob Agents Chemother 1993; 37(9): 1764–70
Pepin J, Saheb N, Coulombe MA, et al. Emergence of fluoroquinolones as the predominant risk factor for Clostridium difficile-associated diarrhea: a cohort study during an epidemic in Quebec. Clin Infect Dis 2005; 41(9): 1254–60
von Baum H, Sigge A, Bommer M, et al. Moxifloxacin prophylaxis in neutropenic patients. J Antimicrob Chemother 2006; 58(4): 891–4
Gaynes R, Rimland D, Killum E, et al. Outbreak of Clostridium difficile infection in a long-term care facility: association with gatifloxacin use. Clin Infect Dis 2004; 38(5): 640–5
Liu HH. Use of the respiratory fluoroquinolones for the outpatient management of community-acquired pneumonia. Curr Ther Res 2004; 65(3): 225–38
Oliphant CM, Green GM. Quinolones: a comprehensive review. Am Fam Physician 2002; 65(3): 455–64
Loo VG, Poirier L, Miller MA, et al. A predominantly clonal multi-institutional outbreak of Clostridium difficile-associated diarrhea with high morbidity and mortality. N Engl J Med 2005; 353(23): 2442–9
Mendez MN, Gibbs L, Jacobs RA, et al. Impact of a piperacillin-tazobactam shortage on antimicrobial prescribing and the rate of vancomycin-resistant Enterococci and Clostridium difficile infections. Pharmacotherapy 2006; 26(1): 61–7
Rubinstein E. History of quinolones and their side effects. Chemotherapy 2001; 47 Suppl. 3: 3–8, discussion 44–8
Andriole VT. The quinolones: past, present, and future. Clin Infect Dis 2005; 41 Suppl. 2: S113–9
Ball P, Stahlmann R, Kubin R, et al. Safety profile of oral and intravenous moxifloxacin: cumulative data from clinical trials and postmarketing studies. Clin Ther 2004; 26(7): 940–50
File TM, Iannini PB. A profile of gemifloxacin, a new respiratory fluoroquinolone. Todays Ther Trends 2003; 21: 415–35
Saravolatz LD, Leggett J. Gatifloxacin, gemifloxacin, and moxifloxacin: the role of 3 newer fluoroquinolones. Clin Infect Dis 2003; 37(9): 1210–5
Owens RC, Ambrose PG. Clinical use of the fluoroquinolones. Med Clin North Am 2000; 84: 1447–69
Mehlhorn AJ, Brown DA. Safety concerns with fluoroquinolones. Ann Pharmacother 2007; 41(11): 1859–66
Shantsila E, Watson T, Lip GY. Drug-induced QT-interval prolongation and proarrhythmic risk in the treatment of atrial arrhythmias. Europace 2007; 9 Suppl. 4: iv37–44
Pollard CE, Valentin JP, Hammond TG. Strategies to reduce the risk of drug-induced QT interval prolongation: a pharmaceutical company perspective. Br J Pharmacol 2008; 154(7): 1538–43
Sanguinetti MC, Jiang C, Curran ME, et al. A mechanistic link between an inherited and an acquired cardiac arrhythmia: HERG encodes the IKr potassium channel. Cell 1995; 81(2): 299–307
Falagas ME, Rafailidis PI, Rosmarakis ES. Arrhythmias associated with fluoroquinolone therapy. Int J Antimicrob Agents 2007; 29(4): 374–9
Kang J, Wang L, Chen XL, et al. Interactions of a series of fluoroquinolone antibacterial drugs with the human cardiac K+ channel HERG. Mol Pharmacol 2001; 59(1): 122–6
Bischoff U, Schmidt C, Netzer R, et al. Effects of fluoroquinolones on HERG currents. Eur J Pharmacol 2000; 406(3): 341–3
Anderson ME, Mazur A, Yang T, et al. Potassium current antagonist properties and proarrhythmic consequences of quinolone antibiotics. J Pharmacol Exp Ther 2001; 296(3): 806–10
Rubinstein E, Camm J. Cardiotoxicity of fluoroquinolones. J Antimicrob Chemother 2002; 49(4): 593–6
Fenichel RR, Malik M, Antzelevitch C, et al. Drug-induced torsades de pointes and implications for drug development. J Cardiovasc Electrophysiol 2004; 15(4): 475–95
Haverkamp W, Breithardt G, Camm AJ, et al. The potential for QT prolongation and proarrhythmia by non-antiarrhythmic drugs: clinical and regulatory implications. Report on a policy conference of the European Society of Cardiology. Eur Heart J 2000; 21(15): 1216–31
Lannini PB, Circiumaru I. Gatifloxacin-induced QTc prolongation and ventricular tachycardia. Pharmacotherapy 2001; 21(3): 361–2
Tsikouris JP, Peeters MJ, Cox CD, et al. Effects of three fluoroquinolones on QT analysis after standard treatment courses. Ann Noninvasive Electrocardiol 2006; 11(1): 52–6
Makaryus AN, Byrns K, Makaryus MN, et al. Effect of ciprofloxacin and levofloxacin on the QT interval: is this a significant “clinical” event? South Med J 2006; 99(1): 52–6
Noel GJ, Goodman DB, Chien S, et al. Measuring the effects of supratherapeutic doses of levofloxacin on healthy volunteers using four methods of QT correction and periodic and continuous ECG recordings. J Clin Pharmacol 2004; 44(5): 464–73
Noel GJ, Natarajan J, Chien S, et al. Effects of three fluoroquinolones on QT interval in healthy adults after single doses. Clin Pharmacol Ther 2003; 73(4): 292–303
Demolis JL, Kubitza D, Tenneze L, et al. Effect of a single oral dose of moxifloxacin (400 mg and 800 mg) on ventricular repolarization in healthy subjects. Clin Pharmacol Ther 2000; 68(6): 658–66
Kahn JB. Quinolone-induced QT interval prolongation: a not-so-unexpected class effect. J Antimicrob Chemother 2000; 46(5): 847–8
Ball P. Quinolone-induced QT interval prolongation: a not-so-unexpected class effect. J Antimicrob Chemother 2000; 45(5): 557–9
Morganroth J, Dimarco JP, Anzueto A, et al. A randomized trial comparing the cardiac rhythm safety of moxifloxacin vs levofloxacin in elderly patients hospitalized with community-acquired pneumonia. Chest 2005; 128(5): 3398–406
Frothingham R. Rates of torsades de pointes associated with ciprofloxacin, ofloxacin, levofloxacin, gatifloxacin, and moxifloxacin. Pharmacotherapy 2001; 21(12): 1468–72
Shaffer DN, Singer SJ. Macrolide antibiotics and torsade de pointes postmarketing analysis [online]. Available from URL: http://www.fda.gov/ohrms/dockets/ac/01/slides/3746s_02_Shaffer/sld001htm [Accessed 2009 Aug 11]
Kessler DA. Introducing MEDWatch: a new approach to reporting medication and device adverse effects and product problems. JAMA 1993; 269(21): 2765–8
Hazell L, Shakir SA. Under-reporting of adverse drug reactions: a systematic review. Drug Saf 2006; 29(5): 385–96
Park-Wyllie LY, Juurlink DN, Kopp A, et al. Outpatient gatifloxacin therapy and dysglycemia in older adults. N Engl J Med 2006; 354(13): 1352–61
Mohr JF, McKinnon PS, Peymann PJ, et al. A retrospective, comparative evaluation of dysglycemias in hospitalized patients receiving gatifloxacin, levofloxacin, ciprofloxacin, or ceftriaxone. Pharmacotherapy 2005; 25(10): 1303–9
Hori S, Kizu J, Kawamura M. Effect of fluoroquinolones on plasma glucose levels in fasted and glucose-loaded mice. J Infect Chemother 2006; 12(2): 109–11
Graumlich JF, Habis S, Avelino RR, et al. Hypoglycemia in inpatients after gatifloxacin or levofloxacin therapy: nested case-control study. Pharmacotherapy 2005; 25(10): 1296–302
Saraya A, Yokokura M, Gonoi T, et al. Effects of fluoroquinolones on insulin secretion and beta-cell ATP-sensitive K+ channels. Eur J Pharmacol 2004; 497(1): 111–7
Lodise T, Graves J, Miller C, et al. Effects of gatifloxacin and levofloxacin on rates of hypoglycemia and hyper-glycemia among elderly hospitalized patients. Pharmacotherapy 2007; 27(11): 1498–505
Gavin IJR, Kubin R, Choudhri S, et al. Moxifloxacin and glucose homeostasis: a pooled-analysis of the evidence from clinical and postmarketing studies. Drug Saf 2004; 27(9): 671–86
McGowan KM, Long SD, Pekala PH. Glucose transporter gene expression: regulation of transcription and mRNA stability. Pharmacol Ther 1995; 66(3): 465–505
Ge TF, Law PY, Wong HY, et al. Gatifloxacin affects GLUT1 gene expression and disturbs glucose homeostasis in vitro. Eur J Pharmacol 2007; 573(1–3): 70–4
Yamada C, Nagashima K, Takahashi A, et al. Gatifloxacin acutely stimulates insulin secretion and chronically suppresses insulin biosynthesis. Eur J Pharmacol 2006; 553(1–3): 67–72
Mohr III JF, Peymann PJ, Troxell E, et al. Risk factors for hyperglycemia in hospitalized adults receiving gatifloxacin: a retrospective, nested case-controlled analysis. Clin Ther 2008; 30(1): 152–7
Ambrose PG, Bhavnani SM, Cirincione BB, et al. Gatifloxacin and the elderly: pharmacokinetic-pharmacodynamic rationale for a potential age-related dose reduction. J Antimicrob Chemother 2003; 52(3): 435–40
Ge DT, Law PY, Kong SK, et al. Disturbance of cellular glucose transport by two prevalently used fluoroquinolone antibiotics ciprofloxacin and levofloxacin involves glucose transporter type 1. Toxicol Lett 2009; 184(2): 81–4
Lewis RJ, Mohr III JF. Dysglycaemias and fluoroquinolones. Drug Saf 2008; 31(4): 283–92
Blayac JP, Hillaire-Buys D, Pinzani V. Fluoroquinolones and anaphylaxis. Therapie 1996; 51(4): 417–8
Sachs B, Riegel S, Seebeck J, et al. Fluoroquinolone-associated anaphylaxis in spontaneous adverse drug reaction reports in Germany: differences in reporting rates between individual fluoroquinolones and occurrence after first-ever use. Drug Saf 2006; 29(11): 1087–100
Johannes CB, Ziyadeh N, Seeger JD, et al. Incidence of allergic reactions associated with antibacterial use in a large, managed care organisation. Drug Saf 2007; 30(8): 705–13
Cutaneous drug reaction case reports: from the world literature. Am J Clin Dermatol 2002; 3 (7): 509–16
Springsklee M, Reiter C, Mayer JM. Safety and tolerability profile of moxifloxacin (MXF) [abstract P0208]. Clin Microbiol Infect 1999; 5 Suppl. 3: 140
Rubinstein E. Safety profile of sparfloxacin in the treatment of respiratory tract infections. J Antimicrob Chemother 1996; 37 Suppl. A: 145–60
_Lipsky BA, Dorr MB, Magner DJ, et al. Safety profile of sparfloxacin in North American phase III clinical trials [abstract no LM-57]. Program and abstracts of the 36th Interscience Conference on Antimicrobial Agents and Chemotherapy; 1996 Sep 15–18; New Orleans (LA). Washington, DC: American Society for Microbiology, 1996
Lee CE, Zembower TR, Fotis MA, et al. The incidence of antimicrobial allergies in hospitalized patients: implications regarding prescribing patterns and emerging bacterial resistance. Arch Intern Med 2000; 160(18): 2819–22
Tilles SA. Practical issues in the management of hypersensitivity reactions: sulfonamides. South Med J 2001; 94(8): 817–24
Nori S, Nebesio C, Brashear R, et al. Moxifloxacin-associated drug hypersensitivity syndrome with toxic epidermal necrolysis and fulminant hepatic failure. Arch Dermatol 2004; 140(12): 1537–8
Iannini P, Mandell L, Felmingham J, et al. Adverse cutaneous reactions and drugs: a focus on antimicrobials. J Chemother 2006; 18(2): 127–39
Roujeau JC, Kelly JP, Naldi L, et al. Medication use and the risk of Stevens-Johnson syndrome or toxic epidermal necrolysis. N Engl J Med 1995; 333(24): 1600–7
Ball P, Mandell L, Niki Y, et al. Comparative tolerability of the newer fluoroquinolone antibacterials. Drug Saf 1999; 21(5): 407–21
De Valle MB, Av Klinteberg V, Alem N, et al. Drug-induced liver injury in a Swedish university hospital out-patient hepatology clinic. Aliment Pharmacol Ther 2006; 24(8): 1187–95
Garcia Rodriguez LA, Stricker BH, Zimmerman HJ. Risk of acute liver injury associated with the combination of amoxicillin and clavulanic acid. Arch Intern Med 1996; 156(12): 1327–32
Perez Gutthann S, Garcia Rodriguez LA. The increased risk of hospitalizations for acute liver injury in a population with exposure to multiple drugs. Epidemiology 1993; 4(6): 496–501
European Medicines Agency. European Medicines Agency recommends restricting the use of oral moxifloxacin-containing medicines [press release]. London: European Medicines Agency Press Office, 2008 Jul 24 [online]. Available from URL: http://www.emea.europa.eu/pdfs/human/press/pr/38292708en.pdf [Accessed 20100 Mar 30]
Fleisch F, Hartmann K, Kuhn M. Fluoroquinolone-induced tendinopathy: also occurring with levofloxacin. Infection 2000; 28(4): 256–7
van der Linden PD, Sturkenboom MC, Herings RM, et al. Fluoroquinolones and risk of Achilles tendon disorders: case-control study. BMJ 2002; 324(7349): 1306–7
Leone R, Venegoni M, Motola D, et al. Adverse drug reactions related to the use of fluoroquinolone antimicrobials: an analysis of spontaneous reports and fluoroquinolone consumption data from three Italian regions. Drug Saf 2003; 26(2): 109–20
van der Linden PD, Sturkenboom MC, Herings RM, et al. Increased risk of achilles tendon rupture with quinolone antibacterial use, especially in elderly patients taking oral corticosteroids. Arch Intern Med 2003; 163(15): 1801–7
Burkhardt O, Kohnlein T, Pap T, et al. Recurrent tendinitis after treatment with two different fluoroquinolones. Scand J Infect Dis 2004; 36(4): 315–6
Committee on Infectious Diseases. The use of systemic fluoroquinolones. Pediatrics 2006; 118(3): 1287–92
Burkhardt JE, Hill MA, Carlton WW, et al. Histologic and histochemical changes in articular cartilages of immature beagle dogs dosed with difloxacin, a fluoroquinolone. Vet Pathol 1990; 27(3): 162–70
Christ W, Lehnert T, Ulbrich B. Specific toxicologic aspects of the quinolones. Rev Infect Dis 1988; 10 Suppl. 1: S141–6
Kato M, Onodera T. Morphological investigation of cavity formation in articular cartilage induced by ofloxacin in rats. Fundam Appl Toxicol 1988; 11(1): 110–9
Grady R. Safety profile of quinolone antibiotics in the pediatric population. Pediatr Infect Dis J 2003; 22(12): 1128–32
Burstein GR, Berman SM, Blumer JL, et al. Ciprofloxacin for the treatment of uncomplicated gonorrhea infection in adolescents: does the benefit outweigh the risk? Clin Infect Dis 2002; 35 Suppl. 2: S191–9
Yee CL, Duffy C, Gerbino PG, et al. Tendon or joint disorders in children after treatment with fluoroquinolones or azithromycin. Pediatr Infect Dis J 2002; 21(6): 525–9
Avalox (Moxifloxacin): summary of product characteristics. Kenilworth (NJ): Schering Corporation, 2006
Tavanic (Levofloxacin) UK package insert. Guildford: Sanofi-aventis, 2006
Ciprofloxacin 2 mg/mL infusion: summary of product characteristics. Kenilworth (NJ): Schering Corporation, 2006
Ciproxin (Ciprofloxacin) tablets 500 mg: summary of product characteristics. Kenilworth (NJ): Schering Corporation, 2008
Stahlmann R, Lode H. Safety considerations of fluoroquinolones in the elderly: an update. Drugs Aging 2001; 27(3): 193–209
Hauser WA, Annegers JF, Kurland LT. Incidence of epilepsy and unprovoked seizures in Rochester, Minnesota: 1935–1984. Epilepsia 1993; 34(3): 453–68
Sannerstedt R, Lundborg P, Danielsson BR, et al. Drugs during pregnancy: an issue of risk classification and information to prescribers. Drug Saf 1996; 14(2): 69–77
Bar-Oz B, Moretti ME, Boskovic R, et al. The safety of quinolones: a meta-analysis of pregnancy outcomes. Eur J Obstet Gynecol Reprod Biol 2009; 143(2): 75–8
Roden DM. Drug-induced prolongation of the QT interval. N Engl J Med 2004; 350(10): 1013–22
Yap YG, Camm AJ. Drug induced QT prolongation and torsades de pointes. Heart 2003; 89(11): 1363–72
Shakeri-Nejad K, Stahlmann R. Drug interactions during therapy with three major groups of antimicrobial agents. Expert Opin Pharmacother 2006; 7(6): 639–51
Ellis RJ, Mayo MS, Bodensteiner DM. Ciprofloxacin-warfarin coagulopathy: a case series. Am J Hematol 2000; 63(1): 28–31
Martin SJ, Sahloff EG, Close SJ. Evaluation and cost assessment of fluoroquinolones in community-acquired respiratory infections. Expert Opin Pharmacother 2002; 3(9): 1251–66
Acknowledgements
Medical writing assistance was provided by Marie Cheeseman, inScience Communications, on behalf of Daiichi Sankyo. This article was supported by Daiichi Sankyo. Hans Liu is on the speakers’ bureaus of Cempra Pharmaceuticals, Cubist, Daiichi Sankyo, Merck, Ortho-McNeil Janssen, Pfizer, Sanofi-aventis and Wyeth, and has received research/ travel grants from Cubist and Ortho-McNeil Janssen.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Liu, H.H. Safety Profile of the Fluoroquinolones. Drug-Safety 33, 353–369 (2010). https://doi.org/10.2165/11536360-000000000-00000
Published:
Issue Date:
DOI: https://doi.org/10.2165/11536360-000000000-00000