Abstract
BACKGROUND: Missed test results are common in clinical practice and compromise patient safety. Direct reporting, whereby testing centers systematically notify both patients and providers of important test results, constitutes a potential solution, but provider acceptance is unknown.
OBJECTIVE: To assess provider interest in direct reporting of selected test results and how interest varied across different tests.
DESIGN, SETTING, AND PARTICIPANTS: Survey of primary care physicians at a tertiary care academic medical center.
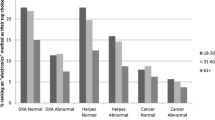
MEASUREMENT: Five-point Likert scores were used to gauge each physician’s interest (1=not at all interested to 5=very interested) in scenarios pertaining to the direct reporting of 3 diagnostic tests of low (DXA scan), intermediate (genital herpes testing), and high (breast biopsy) “emotional impact” and whether interest varied with each test’s result (normal vs abnormal). Physicians were also asked to cite specific advantages and disadvantages of direct reporting.
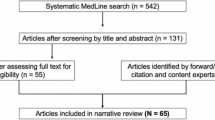
RESULTS: The response rate was 73% (148/202). Physician interest in direct reporting decreased progressively as scenarios shifted from low (DXA scan) to high (breast biopsy) emotional impact (P<.001); interest in direct reporting was also higher when results were normal rather than abnormal (P<.001). Common advantages of direct reporting cited by respondents were reductions in workload (selected by 75% of respondents) and reductions in missed diagnoses (38%). The most common concerns were that patients would become unnecessarily frightened (70%) and would seek unreliable information (65%).
CONCLUSION: Direct reporting of selected test results to patients is one system for insuring that important results are not missed, but implementation should consider the specific test in question, the test result, and provider preferences.
Similar content being viewed by others
References
Hiatt HH, Barnes BA, Brennan TA, et al. A study of medical injury and medical malpractice. New Engl J Med. 1989;321:480–4.
Moore C, Wisnivesky J, Williams S, McGinn T. Medical errors related to discontinuity of care from an inpatient to an outpatient setting. J Gen Intern Med. 2003;18:646–51.
Shields HM, Weiner MS, Henry DR, et al. Factors that influence the decision to do an adequate evaluation of a patient with a positive stool for occult blood. Am J Gastroenterol. 2001;96:196–203.
Roy CL, Poon EG, Karson AS, et al. Patient safety concerns arising from test results that return after hospital discharge. Ann Intern Med. 2005;143:121–8.
Schiff GD, Aggarwal HC, Kumar S, McNutt RA. Prescribing potassium despite hyperkalemia: medication errors uncovered by linking laboratory and pharmacy information systems. Am J Med. 2000;109:494–7.
Schiff GD, Kim S, Krosnjar N, et al. Missed hypothyroidism diagnosis uncovered by linking laboratory and pharmacy data. Arch Intern Med. 2005;165:574–7.
Poon EG, Gandhi TK, Sequist TD, Murff HJ, Karson AS, Bates DW. “I wish I had seen this test result earlier!”: dissatisfaction with test result management systems in primary care. Arch Intern Med. 2004;164:2223–8.
Cram P, Rosenthal GE, Ohsfeldt R, Wallace RB, Schlechte J, Schiff GD. Failure to recognize and act on abnormal test results: the case of screening bone densitometry. Jt Comm J Qual Patient Saf. 2005;31:90–7.
Poon EG, Wang SJ, Gandhi TK, Bates DW, Kuperman GJ. Design and implementation of a comprehensive outpatient results manager. J Biomed Informat. 2003;36:80–91.
Burt CW, Hing E. Use of computerized clinical support systems in medical settings: United States, 2001–03. Adv Data. 2005;353:1–8.
Quality Mammography Standards. Department of Health and Human Services (HHS), Public Health Service (PHS), Food and Drug Administration (FDA). Direct final rule. Federal Register. 1999;64:32404–7.
Priyanath A, Feinglass J, Dolan NC, Haviley C, Venta LA. Patient satisfaction with the communication of mammographic results before and after the mammography quality standards reauthorization act of 1998. Am J Roentgenol. 2002;178:451–6.
Liu S, Bassett LW, Sayre J. Women’s attitudes about receiving mammographic results directly from radiologists. Radiology. 1994;193:783–6.
Lind SE, Kopans D, Good MJ. Patients’ preferences for learning the results of mammographic examinations. Breast Cancer Res Treatment. 1992;23:223–32.
Schreiber MH, Leonard M Jr.,Rieniets CY. Disclosure of imaging findings to patients directly by radiologists: survey of patients’ preferences. Am J Roentgenol. 1995;165:467–9.
Meza JP, Webster DS. Patient preferences for laboratory test results notification. Am J Manag Care. 2000;6:1297–300.
Cram P, Schlechte J, Rosenthal GE, Christensen AJ. Patient preference for being informed of their DXA scan results. J Clin Densitometry. 2004;7:275–80.
Kaushal R, Blumenthal D, Poon EG, et al. The costs of a national health information network. Ann Intern Med. 2005;143:165–73.
Murff HJ, Gandhi TK, Karson AK, Mort EA, Poon EG, Bates DW. Primary care physician attitudes concerning follow-up of abnormal test results and ambulatory decision support systems. Int J Med Informat. 2003;71:137–49.
Baldwin D, Quintela J, Duclos C, Staton E, Pace W. Patient preferences for notification of normal laboratory test results: a report from the ASIPS collaborative. BMC Fam Pract. 2005;6:11.
Hassol A, Walker JM, Kidder D, et al. Patient experiences and attitudes about access to a patient electronic health care record and linked web messaging. J Am Med Informat Assoc. 2004;11:505–13.
Author information
Authors and Affiliations
Corresponding author
Additional information
None of the authors have any conflicts of interest to declare.
Dr. Cram is supported by a K23 career development award (RR01997201) from the NCRR at the NIH.
Rights and permissions
About this article
Cite this article
Sung, S., Forman-Hoffman, V., Wilson, M.C. et al. Direct reporting of laboratory test results to patients by mail to enhance patient safety. J GEN INTERN MED 21, 1075–1078 (2006). https://doi.org/10.1111/j.1525-1497.2006.00553.x
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2006.00553.x