Abstract
CONTEXT: Physician self-disclosure has been viewed either positively or negatively, but little is known about how patients respond to physician self-disclosure.
OBJECTIVE: To explore the possible relationship of physician self-disclosure to patient satisfaction.
DESIGN: Routine office visits were audiotaped and coded for physician self-disclosure using the Roter Interaction Analysis System (RIAS). Physician self-disclosure was defined as a statement describing the physician’s personal experience that has medical and/or emotional relevance for the patient. We stratified our analysis by physician specialty and compared patient satisfaction following visits in which physician self-disclosure did or did not occur.
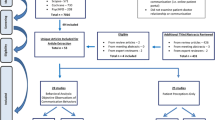
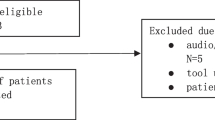
PARTICIPANTS: Patients (N=1,265) who visited 59 primary care physicians and 65 surgeons.
MAIN OUTCOME MEASURE: Patient satisfaction following the visit.
RESULTS: Physician self-disclosure occurred in 17% (102/589) of primary care visits and 14% (93/676) of surgical visits. Following visits in which a primary care physician self-disclosed, fewer patients reported feelings of warmth/friendliness (37% vs 52%; P=.008) and reassurance/comfort (42% vs 55%; P=.027), and fewer reported being very satisfied with the visit (74% vs 83%; P=.031). Following visits in which a surgeon self-disclosed, more patients reported feelings of warmth/friendliness (60% vs 45%; P=.009) and reassurance/comfort (59% vs 47%; P=.044), and more reported being very satisfied with the visit (88% vs 75%; P=.007). After adjustment for patient characteristics, length of the visit, and other physician communication behaviors, primary care patients remained less satisfied (adjusted odds ratio [AOR], 0.45; 95% confidence interval [CI], 0.24 to 0.81) and surgical patients more satisfied (AOR, 2.22; 95% CI, 1.12 to 4.50) after visits in which the physician self-disclosed.
CONCLUSIONS: Physician self-disclosure is significantly associated with higher patient satisfaction ratings for surgical visits and lower patient satisfaction ratings for primary care visits. Further study is needed to explore these intriguing findings and to define the circumstances under which physician self-disclosure is either well or poorly received.
Similar content being viewed by others
References
Roter DL. The Roter Interaction Analysis System (RIAS) Coding Manual. Baltimore, Md: School of Hygiene and Public Health, Johns Hopkins University; 1991.
Gabbard GO, Nadelson C. Professional boundaries in the physician-patient relationship. JAMA. 1995;273:1445–9.
Candib LM. What doctors tell about themselves to patients: implications for intimacy and reciprocity in the relationship. Fam Med. 1987;19:23–30.
Fay A. Boundaries in the physician-patient relationship. JAMA. 1995;274:1345–6.
Lazarus AA. Boundaries in the physician-patient relationship. JAMA. 1995;274:1346.
Frank E, Breyan J, Elon L. Physician disclosure of healthy personal behaviors improves credibility and ability to motivate. Arch Fam Med. 2000;9:287–90.
Levinson W, Roter DL, Mullooly JP, Dull VT, Frankel RM. Patient-physician communication: the relationship with malpractice claims among primary care physicians and surgeons. JAMA. 1997;277:553–9.
Inui T, Carter W, Kukull W, Haigh V. Outcomes based on doctor-patient interaction analysis: I. Comparison of techniques. Med Care. 1982;20:535–49.
Wolraich ML, Albanese M, Stone G, et al. Medical communication behavior system: an interactional analysis system for medical interactions. Med Care. 1986;24:891–903.
Wissow L, Roter DL, Wilson M. Pediatrician interview style and mothers’ disclosure of psychosocial issues. Pediatrics. 1994;13:289–95.
Roter DL, Stewart M, Putnam SM, Lipkin M, Stiles W, Inui TS. Communication patterns of primary care physicians. JAMA. 1997;277:350–6.
Beach MC, Roter D, Larson S, Levinson W, Ford DE, Frankel R. What do physicians tell patients about themselves? A qualitative analysis of physician self-disclosure. J Gen Intern Med. 2004;19:911–16.
Wasserman RC, Inui TS, Barriatua RD, Carter WB, Lippincott P. Pediatric clinicians’ support for parents makes a difference: an outcome-based analysis of clinician-parent interaction. Pediatrics. 1984;74:1047–53.
Donavan JL, Blake DR. Qualitative study of interpretation of reassurance among patients attending rheumatology clinics: “just a touch of arthritic, doctor?” BMJ. 2000;320:541–4.
Frankel RM, Beckman HB. Impact: an interaction-based method for preserving and analyzing clinical transactions. In: Pettegrew LS, ed. Straight Talk: Explorations in Provider and Patient Interaction. Louisville, Ky: Humana.
Beckman HB, Frankel RM. The use of videotape in internal medicine training. J Gen Intern Med. 1994;9:517–21.
Cooper-Patrick L, Ford DE, Vu HT, Power NR, Steinwachs DM, Roter DL. Patient-physician race concordance and communication in primary care. J Gen Intern Med. 2000;15(suppl 1):106.
Smith RC, Marshall-Dorsey AA, Osborn GG, et al. Evidence-based guidelines for teaching patient-centered interviewing. Patient Educ Couns. 2000;39:27–36.
Platt FW, Gaspar DL, Coulehan JL, et al. “Tell me about yourself”: the patient-centered interview. Ann Intern Med. 2001;134:1079–85.
Smith RC, Dorsey AM, Lyles JS, Frankel RM. Teaching self-awareness enhances learning about patient-centered interviewing. Acad Med. 1999;74:1242–8.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by grant 99-504 from the Bayer Institute for Health Care Communication and by grant R01 07289 from the Agency for Healthcare Policy Research.
Rights and permissions
About this article
Cite this article
Beach, M.C., Roter, D., Rubin, H. et al. Is physician self-disclosure related to patient evaluation of office visits?. J GEN INTERN MED 19, 905–910 (2004). https://doi.org/10.1111/j.1525-1497.2004.40040.x
Issue Date:
DOI: https://doi.org/10.1111/j.1525-1497.2004.40040.x