Abstract
Background
Upper gastrointestinal bleeding (UGIB) may present as hematemesis, coffee-ground emesis, or melena requiring esophagogastroduodenoscopy (EGD) for diagnosis and/or therapy. Worldwide, differences exist for the etiology of UGIB reflecting geographical differences in common disease states. In the past 25 years, there have been improvements in endoscopic optics. This study was undertaken to determine: 1) if identifying a bleeding source in UGIB have improved with better endoscopic optics, 2) geographic differences in causes of UGIB, 3) differences in severity of UGIB based on clinical factors, and 4) the likelihood of fi nding a bleeding source based on symptom duration and time to endoscopy.
Methods
A retrospective chart review was made on children having EGD for evaluation of UGIB. Data collected included type, etiology, and degree of bleeding.
Results
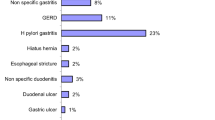
Of 2569 diagnostic procedures, 167 (6.5%) were performed for UGIB. The most common presentation was hematemesis (73.4%). Melena was associated with lower hemoglobin levels and higher transfusion rates. A source of UGIB was found in 57.0%, no cause in 11.4% and a questionable cause in 29.7%. A source was found less commonly in children with a history of UGIB less than one month and in those undergoing endoscopy over 48 hours after a bleeding episode.
Conclusions
Improved endoscopic optics has not changed diagnostic ability for UGIB. Etiologic differences for UGIB in children from varying geographic areas are related to indication for endoscopy, patient selection, and co-morbid conditions. Duration of bleeding and time to endoscopy after a bleeding episode may help predict when endoscopy should be performed to determine a bleeding source.
Similar content being viewed by others
References
El Mouzan MI, Abdullah AM, Al-Mofleh IA. Yield of endoscopy in children with hematemesis. Trop Gastroenterol 2004;25:44–46.
Dehghani SM, Haghighat M, Imanieh MH, Tabebordbar MR. Upper gastrointestinal bleeding in children in Southern Iran. Indian J Pediatr 2009;76:635–638.
Akasaka Y, Misaki F, Miyaoka T, Nakajima M, Kawai K. Endoscopy in pediatric patients with upper gastrointestinal bleeding. Gastrointest Endosc 1977;23:199–200.
Houben CH, Chiu PW, Lau JY, Lee KH, Ng EK, Tam YH, et al. Duodenal ulcers dominate acute upper gastrointestinal tract bleeding in childhood: a 10-year experience from Hong Kong. J Dig Dis 2008;9:199–203.
Huang IF, Wu TC, Wang KS, Hwang B, Hsieh KS. Upper gastrointestinal endoscopy in children with upper gastrointestinal bleeding. J Chin Med Assoc 2003;66:271–275.
Mittal SK. Upper gastrointestinal endoscopy in children. Indian Pediatr 1989;26:134–138.
Mittal SK, Kalra KK, Aggarwal V. Diagnostic upper GI endoscopy for hemetemesis in children: experience from a pediatric gastroenterology centre in north India. Indian J Pediatr 1994;61:651–654.
Quak SH, Lam SK, Low PS. Upper gastrointestinal endoscopy in children. Singapore Med J 1990;31:123–126.
Yachha SK, Khanduri A, Sharma BC, Kumar M. Gastrointestinal bleeding in children. J Gastroenterol Hepatol 1996;11:903–907.
Prolla JC, Diehl AS, Bemvenuti GA, Loguercio SV, Magalhães DS, Silveira TR. Upper gastrointestinal fi beroptic endoscopy in pediatric patients. Gastrointest Endosc 1983;29:279–281.
Ament ME, Christie DL. Upper gastrointestinal fiberoptic endoscopy in pediatric patients. Gastroenterology 1977;72:1244–1248.
Cox K, Ament ME. Upper gastrointestinal bleeding in children and adolescents. Pediatrics 1979;63:408–413.
Liebman WM. Fiberoptic endoscopy of the gastrointestinal tract in infants and children. I. Upper endoscopy in 53 children. Am J Gastroenterol 1977;68:362–366.
Tedesco FJ, Goldstein PD, Gleason WA, Keating JP. Upper gastrointestinal endoscopy in the pediatric patient. Gastroenterology 1976;70:492–494.
Axon AT, Clarke A. Haematemesis: a new syndrome? BMJ 1975;1:491–492.
Byfield F, Ligresti R, Green PH, Finegold J, Garcia-Carrasquillo RJ. Hematemesis due to prolapse gastropathy: an emetogenic injury. Gastrointest Endosc 1998;48:527–529.
Shepherd HA, Harvey J, Jackson A, Colin-Jones DG. Recurrent retching with gastric mucosal prolapse. A proposed prolapse gastropathy syndrome. Dig Dis Sci 1984;29:121–128.
Young GP, Thomas RJ, Wall AJ. Retrograde gastric mucosal prolapse as a cause of haematemesis. Med J Aust 1976;2:488–489.
Thomas E, Khatak KG. Hemorrhage due to retrograde prolapse of stomach. An endoscopic diagnosis. Am J Gastroenterol 1979;71:477–480.
Clemenz FW, Dawson RG. Esophageal dyskinesia and the Mallory-Weiss syndrome. Case report. Arch Surg 1966;93:614–615.
Weaver DH, Maxwell JG, Castleton KB. Mallory-Weiss syndrome. Am J Surg 1969;118:887–892.
Kinsella TJ, Morse RW, Hertzog AJ. Spontaneous rupture of the esophagus. J Thorac Surg 1948;17:613–631.
de Veer AJ, Bos JT, Niezen-de Boer RC, Böhmer CJ, Francke AL. Symptoms of gastroesophageal reflux disease in severely mentally retarded people: a systematic review. BMC Gastroenterol 2008;8:23.
Orchard JL, Stramat J, Wolfgang M, Trimpey A. Upper gastrointestinal tract bleeding in institutionalized mentally retarded adults. Primary role of esophagitis. Arch Fam Med 1995;4:30–33.
Chang CS, Poon SK, Lien HC, Chen GH. The incidence of reflux esophagitis among the Chinese. Am J Gastroenterol 1997;92:668–671.
Kang JY, Tay HH, Yap I, Guan R, Lim KP, Math MV. Low frequency of endoscopic esophagitis in Asian patients. J Clin Gastroenterol 1993;16:70–73.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cleveland, K., Ahmad, N., Bishop, P. et al. Upper gastrointestinal bleeding in children: an 11-year retrospective endoscopic investigation. World J Pediatr 8, 123–128 (2012). https://doi.org/10.1007/s12519-012-0350-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-012-0350-8